MIPS Challenges You Have to Prepare for in 2020
Posted by Jane Kirsty Pardo
Healthcare Technology MIPS MACRA QPP
The Center for Medicaid (CMS) has released the final 2020 Physician Fee Schedule (PFS) with the revised requirements. More participants have received positive payment adjustments since the implementation of MIPS, urging CMS to substantially raise the performance thresholds and data completeness.
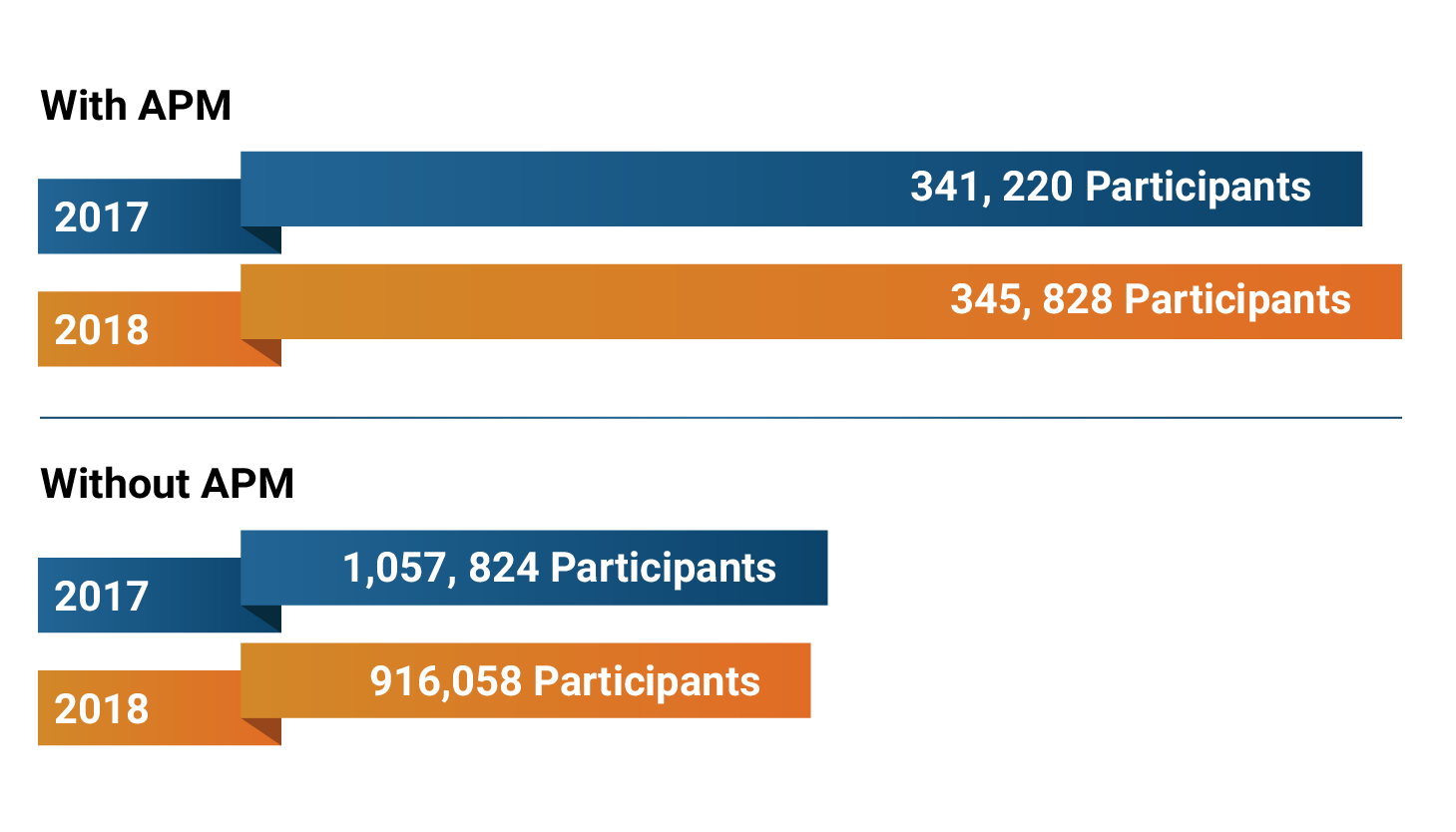
Preliminary MIPS Eligibility


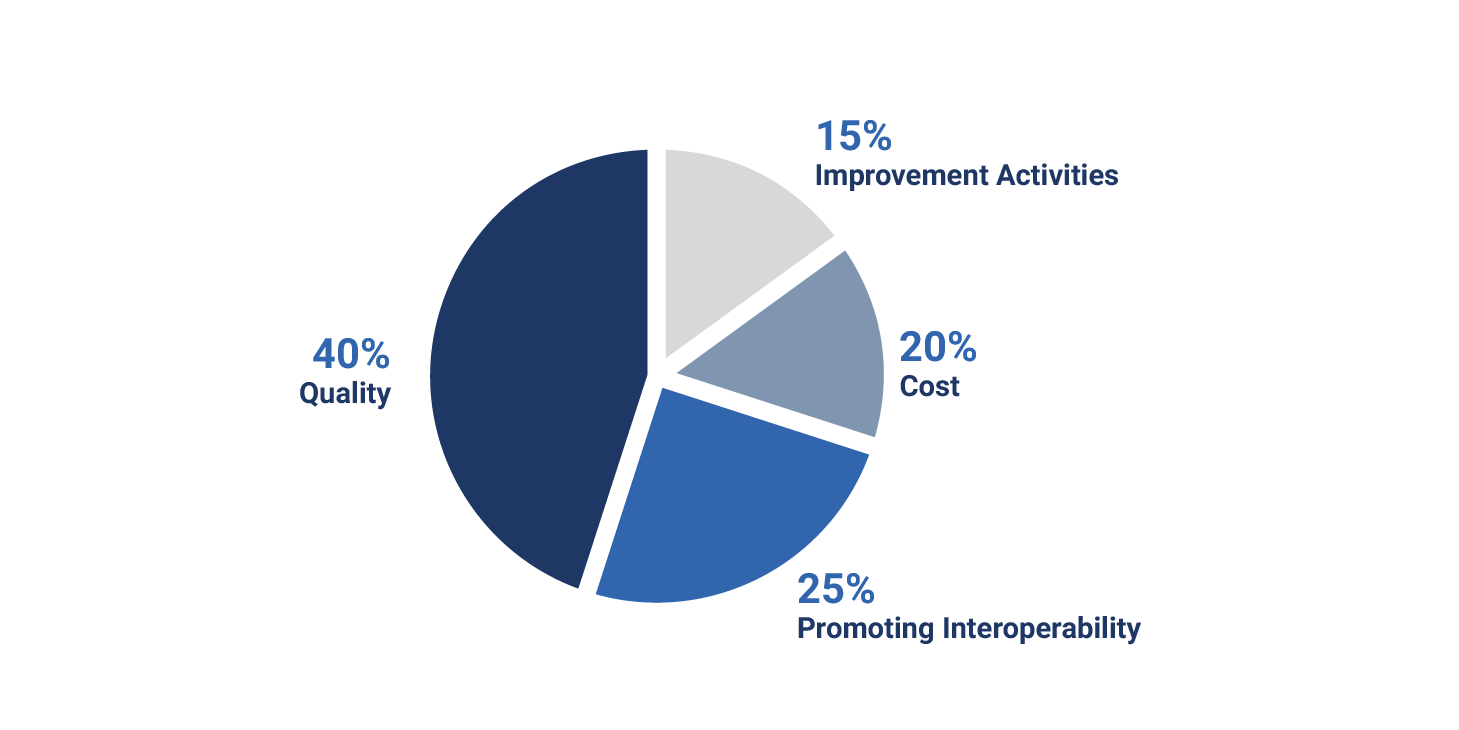
2020 MIPS Category Weights
CMS continues to raise its game to encourage meaningful participation and improve patient outcomes. Substantial adjustments to the rules have been made to achieve these goals. This means that reporting for MIPS may become more challenging every year. Although the previous results are encouraging, some clinicians still have reservations about whether to participate or opt-out of the program. Are you still hesitant, or are you participating this year? Either way, your practice needs to know more about MIPS.
To get you through another reporting year, we’ve listed the challenges you have to prepare for this 2020:
- Difficulty aligning MIPS with your existing workflows
- Unnecessary redundancies and work without the proper tools
- Too many choices when it comes to selecting and reporting on MIPS measures
- The need to have dedicated staff to monitor data and implement quality improvement programs.
- Some measures may feel unattainable

Keeping up with the changing regulatory requirements is not an easy feat, but it can be managed more efficiently with specialized data entry and reporting tools. MIPS reporting features that are integrated with your current EHR system can help you accomplish a successful MIPS submission every year.
MIPS reporting ceases to be a burden with the right software and support. Our flagship EHR software, IMS, helps you meet your specific reporting needs, achieve better clinical outcomes, and maximize your MIPS incentives with the following built-in features:
Avoid the end-of-year rush and save yourself from the hassle! Let our MIPS specialists show you how easy reporting can be with IMS.
Share this post: on Twitter on Facebook on Google+



