Get One-Click Access to the Apollo Guidelines with IMS
Posted by Raffie Sescon
Healthcare Technology New IMS Feature
Getting a treatment or procedure authorized is a time-consuming process that’s becoming a major headache for patients and providers. Clinics spend hours going back and forth, checking whether the authorization request will be approved or denied. As a result, the time it takes for patients to receive much-needed care is increasingly drawn-out.
To remedy this tiresome process, our latest IMS version comes with integrated guidelines for identifying case management and treatment options.
With just one click, you can access the Apollo Managed Care guidelines in the Authorization Tracking and Diagnosis modules. This makes it vastly easier to send the optimal authorization request and diagnose a patient while being assured that you’ll get the authorization approved.
Click a single button in the Authorization Detail window and you’ll immediately receive the applicable codes for your request. Apollo also provides guidelines to help identify health conditions through ICD codes.
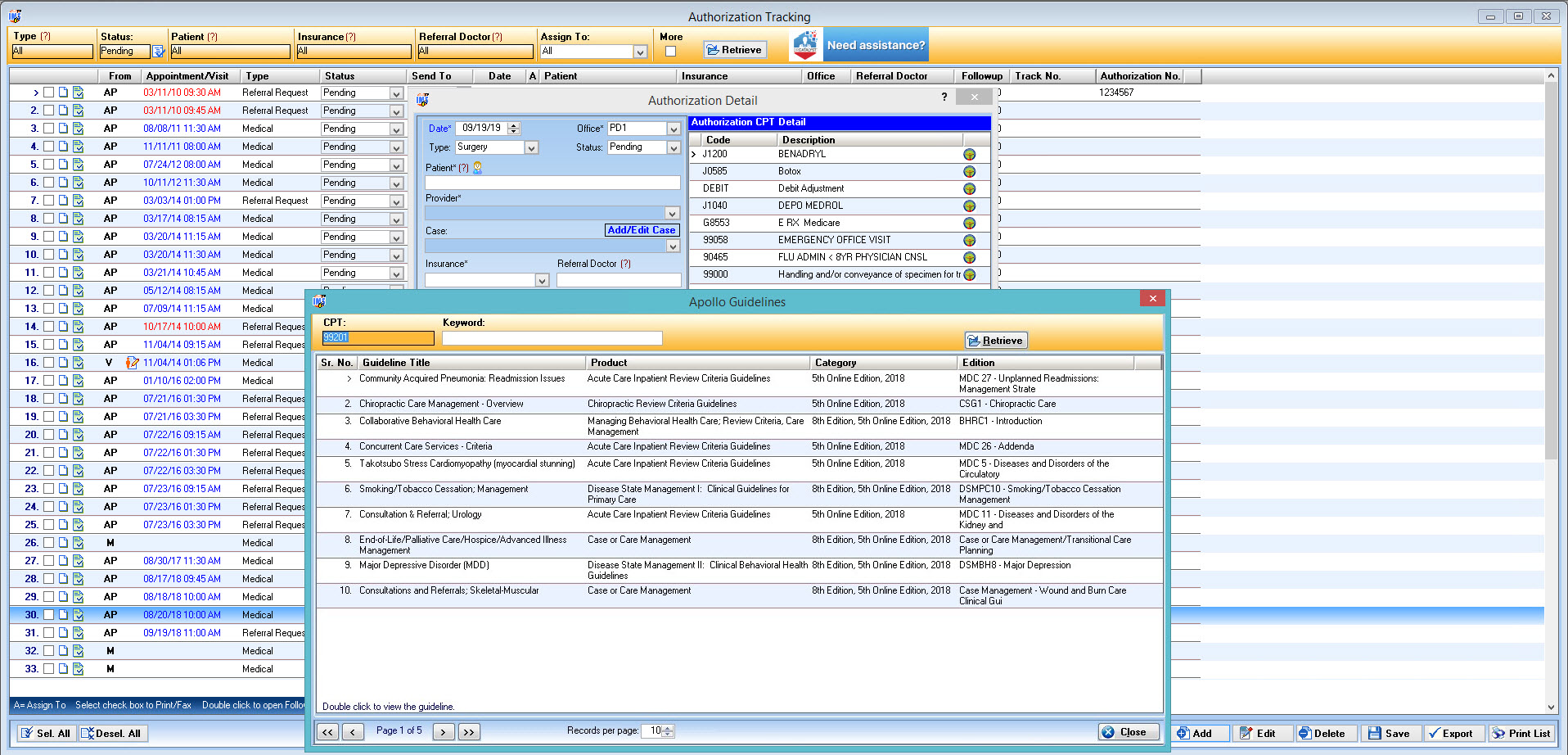
Whether you are billing CPTs, documenting ICDs, or ordering procedures, our integrated Apollo guidelines will be your key card to get your claims right and secure your reimbursements.
Our seamless integration with Apollo Managed Care can be activated in just 2 business days from your activation request. To upgrade to the latest IMS version, contact your account manager at info@meditab.com.
Share this post: on Twitter on Facebook on Google+


